Foot Disorders Patient Information


FOOT SURGERY
The following information is provided as a guide, every patient is different and treatment can be tailored to suit each patient and their individual needs. If you are after a particular type of treatment, please discuss this with your surgeon at the time of your appointment. Please click on the links below to go direct to the information of interest.
BUNION SURGERY
A bunion is a deformity of the great toe related to deviation of metatarsal medially (toward the inside of your foot) while the toe itself deviates laterally (toward the 2nd toe). A bunion can be caused by incorrect footwear, inflammatory arthritis or genetic disposition.
A bunion can be treated either conservatively by adjusting your footwear, or using a spacer to reduce the pressure from rubbing of the big toe on the 2nd toe. If this fails, then your surgeon may recommend surgery to realign the big toe.
The surgery usually involves shaving the bony prominence, performing an osteotomy (controlled cut of the metatarsal), realigning the great toe, adjusting the ligaments and capsule of the joint, then pinning the osteotomy together with screws. Occasionally the bunion deformity can be so severe that it can cause arthritis of the joint, in which case then the only surgical treatment is to correct the deformity and fuse the joint.
Either way, this can usually be done as day surgery, and your surgeon will provide you a rigid soled shoe that you can start weight bearing in on your heel, till the osteotomy heals (usually 6 weeks). There can be residual swelling and bruising to the toe that can take up to a couple of months to resolve.
Keyhole (percutaneous/MIS) Bunion Surgery
Recent advances in bunion surgery now allow us to perform correction of the deformity in the big toe by using small keyhole or percutaneous stab incisions in the skin.
When combined with the use of a specific burr to perform the osteotomy and instruments to shift the toe under x-ray guidance in theatre, good alignment can be achieved, minimising the risk of wound infection and long scars, with similar or accelerated recovery times after surgery.
The correction is still held with 2 screws and you will still be allowed weight bearing in a post op shoe for 6 weeks. In total there will roughly be about 5 small keyhole cuts in your foot.
Common Toe Deformities
- Hammertoe: A Hammertoe deformity occurs when there is flexion of the middle phalanx at the proximal interphalangeal joint (PIPJ) with simultaneous extension of the proximal phalanx. Although it can affect any of the lesser toes, it commonly involves the 2nd toe, mainly due to the 2nd toe being the longest of the lesser toes. Causes can be related to shoewear, previous trauma, inflammatory conditions such as rheumatoid arthritis or neurological conditions.
- Claw toe: The main difference between a claw toe and a hammertoe is that the distal phalanx of the toe can also be flexed downwards, involving the distal interphalangeal joint (DIPJ) as well as the PIPJ. There can also be associated hyperextension at the knuckle of the toe (metatarsophalangeal joint). Similar conditions to the hammertoe can cause a claw toe, though there is more often a neurological condition underlying a claw toe.
- Mallet toe: Similar to a mallet finger, a mallet toe is a deformity only involving the distal phalanx of the lesser toes, causing a flexion of the toe at the DIPJ. These are much less common and usually do not cause as much trouble as the hammer and claw toes.Generally most of these toe deformities can be treated without surgery. A referral to a podiatrist or orthotist for adjustment of wider and higher shoes, or various splints are available to accommodate the deformities. The most common complaints relating to these toes are from rubbing either on the top of the toes at the PIPJ, under the knuckle of the metatarsophalangeal joint, or at the tip of the toe. There can also be associated development of arthritis in the joints from longstanding deformities that can be painful.
- Bunionette (Tailor’s Bunion): A Bunionette deformity is less common and is basically a bunion deformity affecting the little toe. Similar to the big toe bunion deformity (link here), there can be associated rubbing and pain on the outside border of the little toe. Accommodative shoewear can usually fix the problem, otherwise similar to a bunion, corrective surgery can be utilised if all conservative measures have been exhausted.
Plantar Fasciitis
Plantar fasciitis is a degenerative or inflammatory condition affecting the plantar fascia. This is a band that runs under your foot, from its attachment to the heel (calcaneus) where it fans out to extend to all the toes. It is important to maintain the tension and shape of your foot, and works in conjunction with the Achilles tendon to give you good push off power.
Plantar fasciitis is commonly caused by a repetitive strain to the ligament causing micro tears and inflammation, usually at its attachment to the calcaneus under the sole of your foot. This can be attributed to repetitive exercise, poor shoewear, or certain inflammatory arthropathies. Patients typically complain of pain localised on the bottom of your foot, that can radiate from your heel into the arch. It is worse 1st thing in the morning, where it can get better for a while, before prolonged walking or exercise can then bring the pain on again.
These are usually diagnosed with an ultrasound, though sometimes an x-ray will reveal a spur on the bottom of the calcaneus. Though it is a common enough finding, research has shown that the spur (unless very large), typically is not associated with the development or treatment of plantar fasciitis.
It is a difficult problem to treat, though the majority do resolve, with time. It is certainly worth exhausting all non-operative measures prior. These include a soft cushioned heel pad, orthotics with an arch support, plantar fascia massages & stretches and occasionally shock wave therapy. Steroid injections may initially calm down the inflammation, though it is advisable to seek the advice of your surgeon as they can potentially also weaken the plantar fascia causing further tearing.
Surgery is usually a last resort if non-operative measures have failed. Your surgeon will usually perform this through a small cut on the bottom or side of your heel, releasing only a portion of the plantar fascia. This is to ensure the tension & shape of your foot is maintained, but also preventing recurrence. It is usually done as day surgery, and you will be provided with a stiff soled post op shoe to walk on straight away. Typically once the swelling & pain improves after 3-4 weeks you can then mobilise in a comfortable jogger as tolerated.
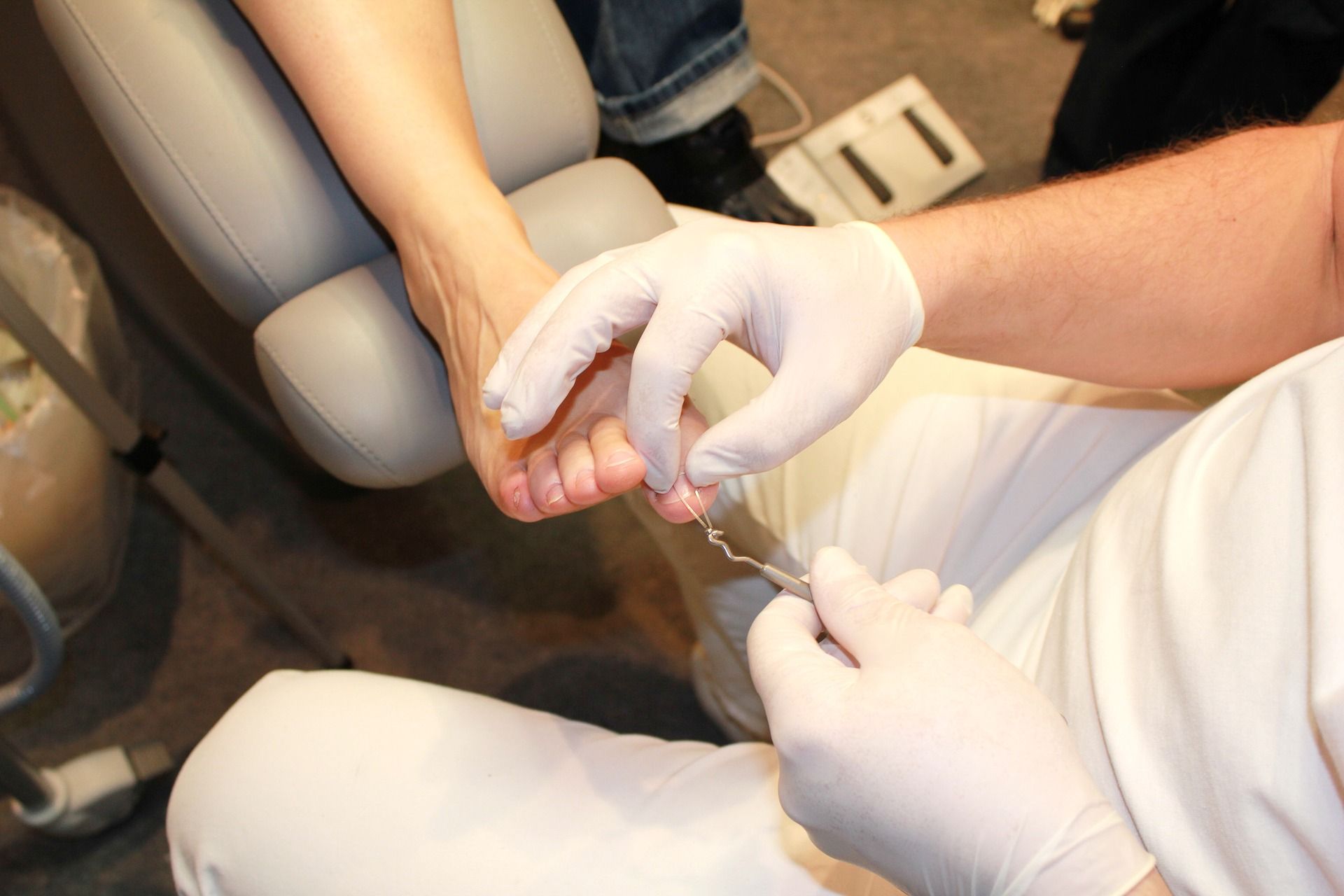
Ingrown Toenails
An ingrown toenail is a common condition that usually affects the big toe. It can cause pain, swelling and progress to recurrent infections. It is commonly caused by inappropriate shoewear, repetitive trauma, incorrect cutting of the toenail or a genetically curved toenail that is predisposes the nail to curl down and grow into the skin.
This can be treated if picked up early enough by gentle soaking of the toe in warm water for 15-20mins, then gently trying to push the skin away from the edge of the toenail, or lifting the toe nail away from the skin edges at the tip with a soft tipped cotton bud.
If this doesn’t work, seeking your GP or a podiatrist can help. Your GP or podiatrist may recommend changes to your shoewear or place you on antibiotics if an infection is suspected. An ingrown toenail can usually be treated successfully in the outpatient setting under local anaesthetic by cutting the edge of the toenail that is ingrown away.
If further surgery is required, it is then important to excise the germinal matrix at the base of the toenail to permanently prevent recurrence or growth of the nail at the edge. Your surgeon may also use a particular chemical called phenol to further prevent growth of the toenail. There may be sutures that will require removal at the 2 week mark, and you will be allowed to weight bear through your foot, but it can take up to 4-6 weeks before the swelling settles such that you can fit yourself into comfortable shoes again.
Mortons Neuroma
A neuroma is a benign growth of nerve tissue forming a painful ball of nerves, commonly affecting the nerves supplying the sensation between the webspaces of the toes.
The most common webspace affected is the 2nd (between the 2nd toe & 3rd toe), however any of the webspaces can be affected, albeit with decreasing frequency.
Causes of a neuroma can be related to the length of toes, a foot with a high arch, improper footwear or repetitive stress/injury to the toes.
The most common symptoms are of pins & needles or numbness between the webspace affected, or the sensation of walking on a pea or stone underneath the foot.
Initially conservative management such as orthotics or a cortisone injection may relieve symptoms, as the nerve initially is only inflamed, and has not yet formed a neuroma, however as time and symptoms progress, surgery may be warranted.
The surgical management of a Mortons neuroma involves excision of the nerve, usually through a cut on the top of the foot. This will cause permanent numbness between the affected webspace, however the rest of the sensation surrounding the toes are preserved, and this will not affect any of your daily activities. Usually this can be done as day surgery, and your surgeon may recommend a stiff soled post op shoe to mobilise on straight away till the swelling settles.
Contact Dr Gerald for details on Early Functional Rehab and Day Surgery
Lisfranc Ligament Tear or Fracture
Lisfranc was a surgeon in Napoleon Bonaparte’s army. The Lisfranc ligament was named after this surgeon, who coined the amputation of the foot with the same name. Soldiers in the army who used to ride horses were thrown off their horses catching and twisting their feet in the stirrups, causing the Lisfranc injury.
These days the Lisfranc ligament can be injured in multiple ways – either in a high velocity injury such as a car accident, in contact sport, or by twisting your foot.
The Lisfranc ligament is very important as it is the main connection between your 1st and your 2nd ray of your foot. Injury to this ligament potentially causes significant instability and can cause ongoing pain & arthritis in future.
Depending on the severity of injury, suspicion for the Lisfranc injury is pain localised in the middle of your foot, bruising that can track through to the bottom of your foot or a “fleck sign” which is avulsion of the Lisfranc ligament on x-ray, with widening between your 1st and 2nd ray.
If you have had a bad twist of your foot and symptoms as described above, touch base with your GP or Orthopaedic Surgeon to have a weight bearing x-ray of your feet, CT or MRI to determine whether the Lisfranc ligament is involved.
A partial injury can be managed with a Moon Boot or plaster for a period of time, however a bad or complete rupture can lead to surgery.